By Aspen Dental
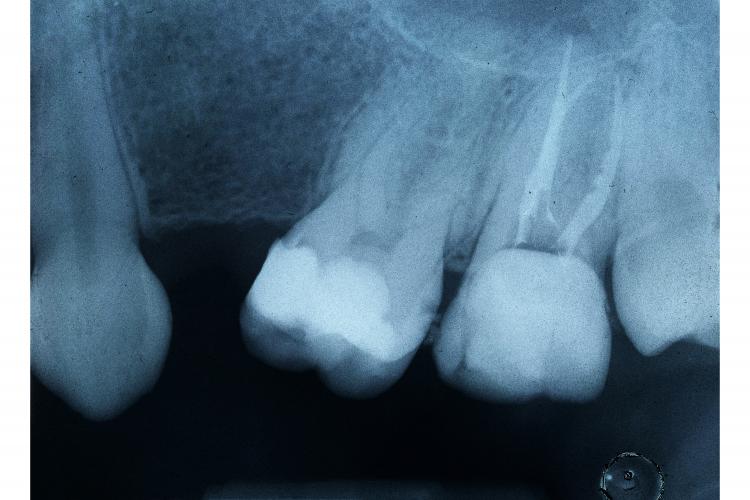
Root Canal
Why Do I Need a Root Canal?
The effects of poor oral hygiene
Proper care of the mouth is extremely significant to the general wellness and overall appearance of an individual. Untreated oral diseases can lead to tooth loss, gum disease, and other dental issues. Dentists and experts believe that there is a link between oral disease and strokes, heart disease, low birth weight, premature births, and diabetes.
Dental diseases are comprised of the following groups:
- diseases of the teeth (formation of cavities and tooth decay)
- gum/periodontal diseases
- mouth sores
- tooth sensitivity
- oral cancer
While dental problems can be distressing, they can be treated and easily prevented. Root canal treatment remains a feasible option for restoring and preserving an otherwise sound tooth.
What are Root Canals?
A root canal is a structural expansion within the root of a tooth. It is part of an innately occurring space within the tooth and consists of the pulp chamber (a hollow part in the center of the tooth that contains the pulp).
The pulp is soft matter located in the center of the tooth and is made of complex anatomical tributaries such as blood vessels, nerves, and connective tissue that link the root canals to the surface of the root and to each other.
When is a Root Canal Treatment Necessary?
Sometimes, the pulp and soft tissue inside the root canal can be infected by bacteria, which can cause inflammation. This can be due to various causes such as the following: a crack or chip in the tooth, an injury to a tooth, repeated dental procedures on the tooth, or deep decay. If the infection or inflammation is left untreated, it can cause serious pain or lead to an abscess (a pus-filled pocket that forms at the end of the roots of the tooth). It is imperative to consult a dentist or endodontist immediately if you start feeling discomfort in your teeth. An endodontist is a dentist who specializes in the causes, diagnosis, prevention, and treatment of injuries and disease of the dental pulp or the nerve of the tooth.
Root canal treatment is a subset of endodontic treatment which deals with defects inside the tooth. This treatment is necessary when the following signs are noticed: swelling, pain (with intensity ranging from mild to severe), discoloration of the tooth, prolonged sensitivity to heat or cold, tenderness to touch and chewing, and drainage and tenderness (in the lymph nodes, bones, and gum tissues).
Elaborating on these symptoms, a toothache is a cardinal pointer for needing a root canal. The pain is usually fairly specific and if the tooth is still alive, the individual affected will experience extreme sensitivity to hot or cold foods or liquids and the sensitivity will continue even after the hot or cold stimulus has stopped. The tooth may start to hurt involuntarily at night, or even when the tooth is not actively used for eating or chewing. The pain can progress to severe generalized headaches. If the tooth is dead and presenting an abscess, then the pain will be felt when pressure is put on the tooth. The abscess may or may not produce bleeding or swelling around the tooth, and sometimes visible swelling of the jaw, cheek, or throat. If this swelling is noticed, treatment is required urgently.
Concerning an abscess, pus accumulates in an area of dead nerve tissue infected with bacteria. Sometimes the abscess will form a bump that resembles a pimple on the exterior part of the gums. You may even notice pus draining from a pimple or notice a bad taste your mouth. If left untreated, it will continue to grow and infect the bone and tissues around the root of the tooth. Although antibiotics minimize the rate at which the infection spreads, the only way to stop the infection completely is by undergoing a root canal treatment. Trauma to the tooth can rip the nerves at the end of the root causing them to die. Also, a tooth that has been fractured may need a root canal if the fracture stretches deep into the tooth and reaches the pulp. Occasionally, repeated dental procedures can produce significant stress on a tooth causing inflammation, which in turn requires a root canal treatment.
An infection may also cause swelling that may spread to other areas of the face, neck, or head to include bone loss around the tip of the root and drainage problems extending outward from the root. A hole can occur through the side of the tooth with drainage into the gums, or through the cheek with drainage into the skin. Although other conditions of the mouth could masquerade as a toothache, sometimes symptoms are not noticed. Therefore, it is very important to get a thorough examination with pulp vitality testing by a licensed dentist for a proper diagnosis, undergo proper routine check-ups, practice good oral hygiene, and avoid chewing on extremely hard foods.
What happens during a root canal treatment?
While undergoing the procedure, the dentist will remove the infected pulp, cautiously clean and shape the interior part of the root canal, and then fill and seal the space with a rubber-like material called gutta-percha. Consequently, you are required to return to the dentist who will place a crown on the tooth to secure and restore it to full function. After this, the tooth can continue to function properly.
The following is expected during the procedure:
X-Ray Technology
An x-ray is used to observe the form and shape of the root canals, determine if there are any signs of infection in a surrounding bone, and locate the decay.
Anesthesia
With modern anesthetics, the procedure can be completely painless. The dentist will use local anesthesia such as lidocaine to numb the area near the tooth.
Pulpectomy
Thirdly, the area is kept dry and free of saliva during treatment by placing a rubber dam around the tooth. A hole to will then be drilled into the tooth to access the pulp. The infected pulp, the dead nerve tissue, and other debris are removed from the tooth. Root canal files are then used to clean the tooth. With increasing diameter of these files, each is subsequently placed into the hole and worked down the full length of the tooth to scrape and scrub the sides of the root canals. Resulting debris is washed away in intervals with various irrigants to clean and kill any remaining bacteria.
Filling
After the tooth is properly cleaned, it is sealed. Your dentist may prefer to wait a week before sealing the tooth in some circumstances. For example, in the case of an infection, the dentist may place a medication inside the tooth to clear it up. Or, your dentists might decide to seal the tooth the same day it is cleaned out. If the root canal is not intact on the same day, a temporary filling is put in the exterior hole in the tooth to keep contaminants like saliva and food from entering the tooth during appointments. Finally, for the interior hole to be filled, a rubber compound called gutta percha and sealer paste is then placed into the root canal. To fill the external hole created at the onset of the treatment, a filling is placed. It is advisable to minimize chewing on the tooth under repair to avoid recontamination of the tooth’s interior and also prevent it from breaking prior to full restoration.
Restoration
A crown is usually placed over the tooth to protect it from damage during the rehabilitation process.
A root canal treatment may require subsequent visits to your dentist or endodontist.
What is the Success Rate of a Root Canal Treatment?
Root canal treatments are rated highly successful with more than a 95% success rate. A tooth with a well-treated root canal restorations can last for many years and possibly a lifetime. Although there is no substitute for your natural teeth, root canal treatment is a viable and sometimes necessary solution.
What is the Cost of a Root Canal Treatment?
The cost of root canal treatment can vary depending on how severe the case is. Contact our office today for an estimate.
What Should I Do After My Root Canal?
Although most patients can return to their normal activities the next day, some for the first few days after completion of the procedure may experience tooth sensitivity as a result of natural tissue inflammation, particularly if there was infection or pain prior to the procedure. This soreness can be controlled with over-the-counter pain medications such as naproxen (Aleve) or ibuprofen (Advil, Motrin).
The most crucial thing to make a root canal last as long as possible is to get the lasting restoration (fillings or crowns) on the tooth immediately after the root canal and maintain that restoration with perfect hygiene. Avoid chewing ice as this can lead to permanent damage, putting small cracks in the enamel. These cracks have the ability to grow larger over time and ultimately cause a tooth fracture, requiring a visit to the dentist and unnecessary expense to get the cracks fixed over again. Deep decay, new trauma or a loose, cracked or broken filling can create new infections in the tooth.
Concerning oral health care, you are advised to brush properly, floss, and use an antiseptic mouthwash as you subsequently see your dentist at scheduled intervals to check the tooth for other signs of failure or reinfection.
Check out these related articles!
About Root Canals
Root Canal Quick Facts: Part 1
Root Canal Quick Facts: Part 2

